Warning Signs of Gum Disease
Gums that bleed easily.
Red, swollen, tender gums.
Gums that have pulled away from the teeth.
Persistent bad breath or bad taste.
Permanent teeth that are loose or separating.
Any change in the way your teeth fit together when you bite.
Any change in the fit of partial dentures.
Studies indicate that upwards of 75% of adults have some level of gum disease. Silent, like diabetes or high blood pressure, gum disease gradually erodes the bone that holds and supports your teeth in the jawbone.
Contact Us
"*" indicates required fields
Stages of Gum Disease

Healthy
Health
Healthy
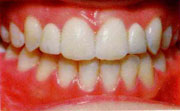
- Coral pink
- Gums tight
- No bleeding
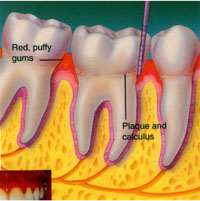
Gingivitis
Mild
Gingivitis
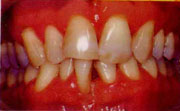
- Bleeding
- Inflamed
- Sensitive
- Bad Breath
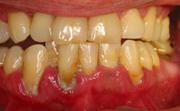
Perio
Moderate
Perio

- Bleeding
- Swelling
- Gums Loosen
- Bad Breath, Taste
- Pockets 4mm

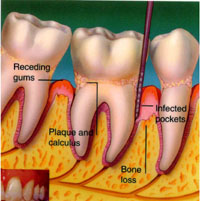
Perio
Advanced
Perio
- Heavy Bleeding
- Swelling
- Recession
- Teeth Loose
- Bad Breath taste
- Pockets 6mm
Diagnosing Gum Disease
A diagnosis is confirmed or ruled out by using a panoramic or full series of radiographs and comparing them with periodontal pocket measurements. During your gum exam, we will use a tiny ruler to measure the depth of the pockets and, at the same time, note any abnormalities like bleeding, pus, gum recession or loose teeth. Those measurements combined with imaging indicate the health of your gum and bone.
Treating Gum Disease
There is no cure for gum disease. The goal of treatment is to eliminate the bacteria causing the disease. We have a comprehensive program called Soft Tissue Management in place. It consists of a full range of non-surgical options as the first line of treatment. Our experts at Matthews dental office will thoroughly guide you about your gum health. If your disease is beyond the scope of nonsurgical care alone, we will most likely refer you to a gum specialist called a periodontist for a precise Periodontal Treatment.

SRP
Scaling and root planing is a detailed cleaning that removes tartar under the gum line and smooths the roots to keep them clean. Usually, we will use a local anesthetic like Oraqix to numb the areas that will be cleaned. Both specialized ultrasonic tips and very fine hand scalers are used to clean deep areas. It will usually take several visits to do a thorough job. If you address your gum disease before it becomes severe, scaling and root planning may be the only treatment you need. However, as with any dental procedure, after-care is vital. In order to keep your teeth in good shape and resist future occurrences of gum disease, you must brush and floss daily, eat a healthy diet, avoid tobacco use, and have regular dental checkups. Even after a successful scaling and root planning, if you don’t attend to your teeth properly, it’s quite likely that you’ll develop gum disease again.

Antibiotics
We have many options available for agents that kill bacteria and assist your body in healing your gums and bone. From tiny local applications that are placed directly in the pocket where the infection hides to rinses and systemic options. Antibiotics have been shown to enhance the results of scaling.

Homecare
There is no cure for periodontal disease. Our goal is to stabilize it and prevent additional bone loss. If you rebuild the engine in your car, you will need to do regular maintenance in order to keep it running. In the same way, you will need to work extra hard at home to keep your teeth clean and come in for professional cleanings several times a year to keep gum disease from coming back.
Surgical Options
If the tissue or bone surrounding your teeth is too damaged to be repaired with non-surgical treatment, several surgical procedures are available to prevent severe damage and restore a healthy smile. Following is a list of common types of periodontal surgery:
Pocket Depth Reduction
In a healthy mouth, the teeth are firmly surrounded by gum tissue and securely supported by the bones of the jaw. Periodontal disease damages these tissues and bones, leaving open spaces around the teeth that we call pockets. The larger these pockets are, the easier it is for bacteria to collect inside them, leading to more and more damage over time. Eventually, the supportive structure degrades to the point that the tooth either falls out or needs to be removed. During pocket reduction procedures (also known as “flap surgery”), we fold back the gum tissue and remove the bacteria hiding underneath, as well as the hardened plaque and tartar that have collected. We may also remove any tissue that is too damaged to survive. We then sew the healthy tissue back into place. Now that the tooth and root are free of bacteria, plaque, and tartar, and the pockets have been reduced, the gums can reattach to the teeth.
Regeneration
When the bone and tissue supporting the teeth have been lost due to severe gum disease, we can restore these areas with a regeneration procedure. During this process, we begin by folding back the gum tissue and removing the bacteria, plaque, and tartar. Depending on your situation, we may then perform a bone graft to stimulate new bone growth, or we may apply a special kind of protein that stimulates tissue growth to repair the areas that have been destroyed by the disease.
Soft-Tissue Graft
A frequent symptom of gum disease is gum recession (also called gingival recession). As the gums recede, more of the roots are revealed. This can make teeth appear longer and can also create sensitivity to hot or cold liquids or food. It also exposes the tooth to increased damage from gum disease, as bacteria, plaque, and tartar attack the surface of the tooth and the root. During a soft-tissue graft, tissue from the top of your mouth or another source is sewed to the gum area, covering the roots and restoring the gum line to its original, healthy location. This procedure can also be performed for cosmetic reasons.